What is the CMS ASPIRE Model? A 10-Year Value-Based Care Roadmap for Digital Health
The Centers for Medicare & Medicaid Services (CMS) is fundamentally shifting the landscape of pediatric care through the Accelerating State Pediatric Innovation Readiness and Effectiveness (ASPIRE) Model. Announced in March 2026, this 10-year, voluntary initiative moves away from fragmented Fee-For-Service (FFS) reimbursement toward a whole-person, Value-Based Care (VBC) framework specifically for children and youth up to age 21 in Medicaid and CHIP.
Why is CMS Focusing on Pediatric Value-Based Care?
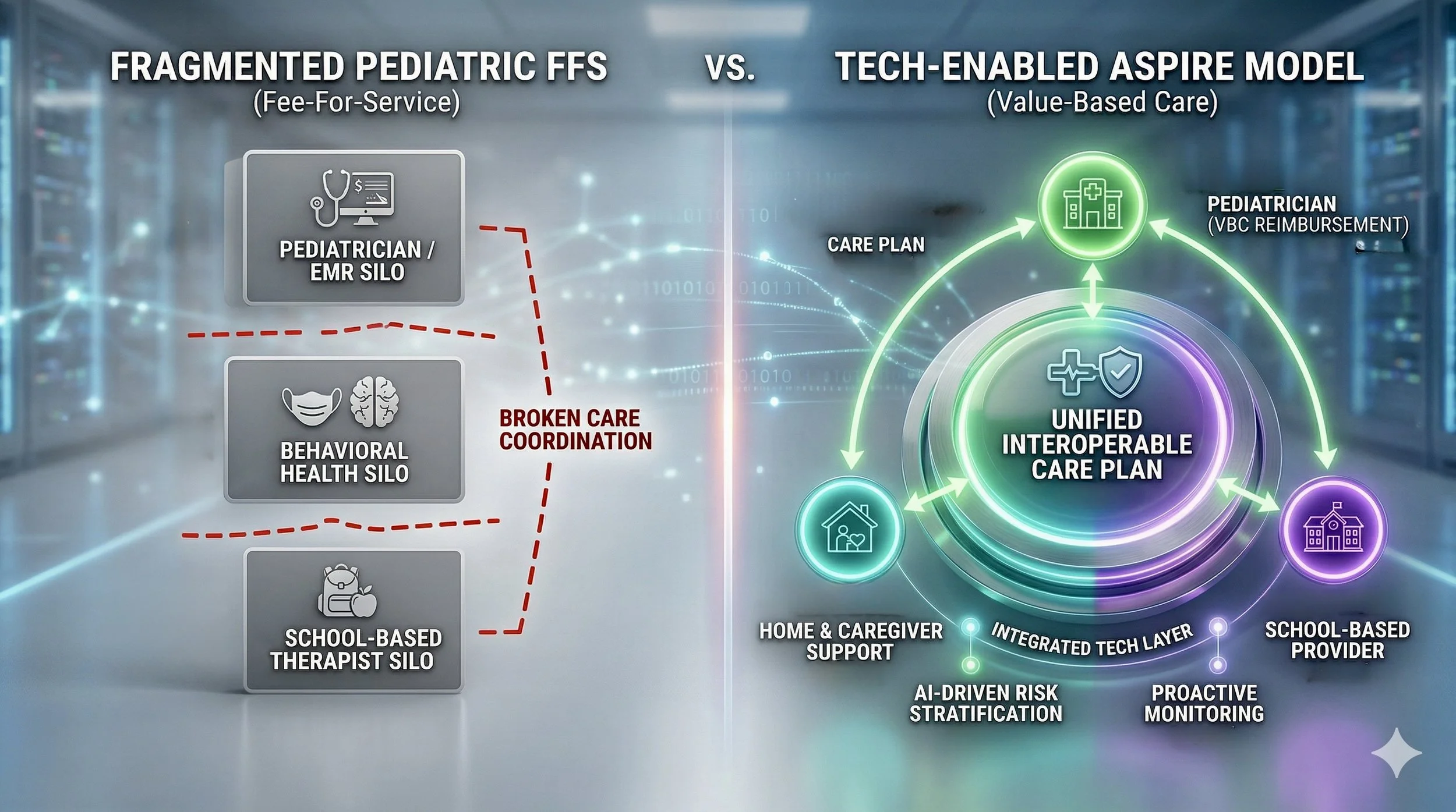
While value-based care (VBC) models are prevalent across the 65+ Medicare population, pediatric care has historically remained rooted in fee-for-service (FFS) models. Traditional FFS reimbursement rarely incentivizes the intensive coordination required to manage children with complex needs, leading to siloed intervention and high system costs. ASPIRE is designed to replace these silos with a "tech-enabled safety net" that rewards organizations for improving whole-person outcomes, not just delivering a volume of "sick care" services.
How Does the ASPIRE Model Work?
The ASPIRE model is a state-based initiative. CMS will select up to five State Medicaid Agencies (SMAs) via Cooperative Agreements, providing funding starting in 2026.
Accountability for Care: These SMAs must partner with Accountable Entities, such as Managed Care Plans or Accountable Care Organizations (ACOs).
Total Cost and Quality: These partner organizations assume accountability for the total cost and quality of care for the enrolled pediatric population, moving away from FFS reimbursement dynamics.
What Are the Technology and Care Requirements for ASPIRE?
To participate in the ASPIRE ecosystem, digital health companies must provide the critical technological "connective tissue" to align pediatricians, behavioral health specialists, and school-based providers. The model prioritizes four core components:
A Unified Care Plan: ASPIRE requires platforms that enable a single, comprehensive care plan shared across the entire care team. It must ensure that a child’s psychiatrist, pediatrician, and school-based therapists are all aligned on progress.
Interoperable Care Management: There is a crucial demand for interoperability solutions that can bridge the significant data gaps between clinical EMRs, school environments, and home-based care.
AI-Driven Proactive Intervention: Solutions must enable proactive monitoring to keep children in the "least restrictive setting" possible. Successful models will leverage AI for risk stratification—analyzing Medicaid datasets to identify "rising risk" children early, allowing prioritization of interventions before conditions escalate into costly crises.
Caregiver Support & Empowerment: ASPIRE emphasizes providing digital tools that empower parents and caregivers, who often spend hours coordinating complex care tasks without professional support.
Key Takeaways
The ASPIRE model is a state-based CMS initiative launched in 2026 to improve outcomes for age 0-21 Medicaid/CHIP beneficiaries with complex medical or behavioral needs. Over its 10-year span, the model utilizes state cooperative agreements and Accountable Entities to transition pediatric care to value-based models, prioritizing interoperability, unified care plans, and proactive intervention.
Contact Nixon Law Group Today
Transitioning to pediatric value-based care requires sophisticated regulatory, privacy, and contracting strategies. Reach out to our team to develop your regulatory strategy and value-based contracting arrangements.
Frequently Asked Questions about the ASPIRE Model
Which patients are eligible for the ASPIRE model?
ASPIRE targets patients up to age 21 enrolled in Medicaid and CHIP who have, or are at risk of developing, complex medical and behavioral health conditions.
When does the CMS ASPIRE Model start?
CMS will select State Medicaid Agencies via cooperative agreements in 2026, initiating a 10-year model run.
Does the ASPIRE model require school-based care coordination?
Yes. A core element of the ASPIRE requirement is a unified care plan accessible and shared by pediatricians, behavioral health specialists, and school-based providers.